What If Beddoes & Davy Had Attempted Surgical Anesthesia In 1799?
Technology’s Stories vol 3, no. 1 – doi: 10.15763/JOU.TS.2015.4.1.01
PDF: Wright_What If Beddoes and Davy
The inhalation of gases to relieve pain during surgery is considered one of America’s greatest contributions to medicine. The “discovery” of anesthesia is often credited to Boston dentist William Morton, who brought an inhalation device and ether into the operating room of Dr. John Collins Warren one October morning in 1846. This event was considered a success—Warren famously declared “Gentlemen, this is no humbug!”—and the “public” demonstration at Massachusetts General Hospital [MGH] meant that within months this new medical development reached various parts of the U.S., Britain and France. Within a year use of ether anesthesia for surgical pain relief had spread to many other countries.
As often happens with technological, scientific, and medical developments, Morton stood on the shoulders of giants to reach that moment in Boston. The trail included numerous individuals who came tantalizingly close to surgical anesthesia, used the wrong agent, or actually achieved it but did not promote their work. Morton was nothing if not a self-promoter. Let’s work backwards on this trail. We can approach these events as a tale of missed opportunities, replete with “what if” scenarios. This excursion also reminds us that innovation seldom follows a lineal progression. By exploring earlier experiments with anesthesia, we see the crucial roles of social contexts in shaping specific medical practices—as well as larger conceptions of medicine itself.
“Thomas Beddoes by Bird” by Pencil drawing by Edward Bird (1772–1819) -http://wellcomeimages.org/indexplus/image/V0000437.html. Licensed under CC BY 4.0 via Wikimedia
Another Boston dentist, Horace Wells, had actually attempted a surgical anesthesia demonstration at MGH in January 1845 with Warren, one of America’s best known surgeons of the day, also presiding. Wells used nitrous oxide, which did not provide as deep a state of unconsciousness as ether. The patient moved and groaned, and the audience of mainly medical students hooted Wells from the operating theater. The patient later stated he had felt no pain.
On March 30, 1842, a physician in Jefferson, Georgia, Crawford Long, used ether on a patient while he removed a neck tumor. Over the next few years Long used ether in other surgeries and in his obstetrical practice but made no effort to announce his discovery to the world. In December 1849, when Morton, Wells and Morton’s mentor Charles Jackson were embroiled in debates over who “discovered” anesthesia, Long finally published his results.
In January 1842 William E. Clarke, a medical student in Massachusetts, used ether to provide pain relief while he removed a tooth from the sister of a classmate. Clarke’s medical school preceptor discouraged further attempts. In the 1820s English physician Henry Hill Hickman used carbon dioxide to provide pain relief in dogs during amputations. Right idea, wrong agent.
Now we come to Thomas Beddoes and Humphry Davy. In 1798 physician Beddoes opened his Pneumatic Institution in Clifton, just outside Bristol, England, after several years of planning. Since the early 1790s Beddoes had been experimenting with various gases in hopes of applying them therapeutically in patients with consumption and other respiratory ailments. He had also been raising money for his institute.
In October 1798 his newly hired research director, Humphry Davy, joined Beddoes in the effort. The Institution would provide clinical care, teaching and research, an unusual combination for the time. Clinical care and teaching might be combined in medical schools, if faculty members allowed students to shadow them on private patient visits or follow them as they made rounds of their patients at a local charity hospital. Research collaboration might consist of the scientist and an assistant, or even his wife as in the case of Lavoisier. Large teaching hospitals where research might also be done or the medical school-hospital-research faculty combination were many decades in the future.

“Humphry Davy Engraving 1830” by unknown, based on a portrait by Sir Thomas Lawrence (1769 -1830
Davy embarked upon a bold research effort, trying many different gases on himself as he searched for ones that could be useful in Beddoes’ search for therapeutic gases. At one point he nearly killed himself. Finally he tried nitrous oxide and found what they hoped would be the perfect gas to use as a medicine on consumptive patients. Using equipment designed by James Watt and others, Davy and Beddoes spent hours each day breathing vast amounts of nitrous oxide. They were joined at various times by individuals present in Bristol and part of Beddoes’ circle: Samuel Taylor Coleridge, Robert Southey, Peter Mark Roget and others as well as many patients at the Institution. Novelist Maria Edgeworth and publisher Joseph Cottle were among the observers.
Davy detailed all of this laboratory and clinical research in a book of 580 pages published in the summer of 1800. By that time the efforts at the Pneumatic Institution had become notorious and the subject of great ridicule by Beddoes’ political enemies. During the 1790s Beddoes had attracted attention for his support of foreign revolutions, and several satiric poems had specifically attached his medical and scientific work. Davy’s book was his summation before escaping Bristol for London and the new Royal Institution where he would become the greatest scientist of his age.
Davy’s book is a painstaking account of the gas work at the Institution, detailed and profusely illustrated. His introduction opens by noting about nitrous oxide, “I was induced to carry on the following investigation concerning its composition, properties, combinations, and mode of operation on living beings.” Davy tested the gas on numerous “living beings” including insects, fish, and various mammals before trying it on himself, other volunteers, and patients at the Institution. His table of contents runs to eight pages.
The final section adds something special to the laboratory and clinical accounts. Many of the people who came and breathed nitrous oxide provided Davy with their subjective accounts of the experience. Future Poet Laureate Robert Southey had a typical reaction: “The atmosphere of the highest of all possible heavens must be composed of this gas.” Davy also discusses his own mental reactions.
During one of those experiments with nitrous oxide, Davy noted that breathing it relieved the pain of a toothache. And near the end of his vast book, on page 556, he tosses out this observation: “As nitrous oxide in its extensive operation appears capable of destroying pain, it may probably be used with advantage during surgical operations in which no great effusion of blood takes place.”

Title page of Davy’s book Source: Wood Library-Museum of Anesthesiology
The mind boggles. Here it is in 1800, the specific idea of surgical anesthesia and some research efforts sufficient to warrant further work. What happened? Why didn’t Beddoes and Davy pursue the idea into actual surgical practice? Anesthesia historians have chewed that bone for a long time.
Some have suggested that changed Western attitudes toward pain, helped by the Romantic Movement, had not yet occurred. Beddoes, who followed Lavoisier’s innovations, thought the future of medicine lay in chemistry, and chemistry was a “French” science” and thus suspect to many in Britain. Beddoes also theorized that surgical pain was no different from pain caused by consumption or other diseases. Britons of this era demonstrated a general callousness toward pain relief. Most believed, for religious or other reasons, that banishment of pain on a consistent basis was impossible. Beddoes and Davy knew that blood conveyed gases and thought blood loss would negate gas effects—thus Davy’s caveat about surgery “in which no great effusion of blood takes place.” On a practical level, the makeshifts in their equipment — made of silk, wood and leather — would have proven inadequate for daily use in surgery, let alone in conditions on a battlefield or at sea.
Beddoes was a physician, not a surgeon—those individuals in Britain were still tradesmen at the time. He did not see surgical intervention as a solution to medical problems. Rather, Beddoes followed the theories of John Brown, a Scottish physician who felt that diseases were the result of too much or too little excitability in the physiological system. Beddoes felt he could apply gases to help increase that excitability where needed.
As we know from his subsequent career, Davy was more interested in chemistry than medicine. And as I’ve noted, the Bristol gas experiments had become notorious and a source of poetic and other satire by the time Davy left for London. The Pneumatic Institution proved to be a dead end; Beddoes spent the remaining few years of his life treating the poor at his clinic.
Despite Beddoes’ own sense of failure, in retrospect we can see that efforts at the Pneumatic Institution hinted at today’s scientific medicine. The facility’s stated purpose involved clinical care, education, and research — a forerunner to today’s academic medical center. Davy did extensive laboratory and animal research on nitrous oxide and discovered that animals lived longer when the gas was mixed with oxygen. He also investigated lung volume via experiments on himself; he was the first human to breath nitrous oxide. Previously the gas, discovered by Joseph Priestley, had been associated with the Doctrine of Septon developed by New York City physician Samuel Latham Mitchill. That philosophy recognized the importance of oxygen, but declared “Septon” as the principle of dissolution. When the two mixed, noxious fume resulted that led to yellow fever and other diseases. In order words, nitrous oxide was believed to be poisonous at the time Davy tried it.
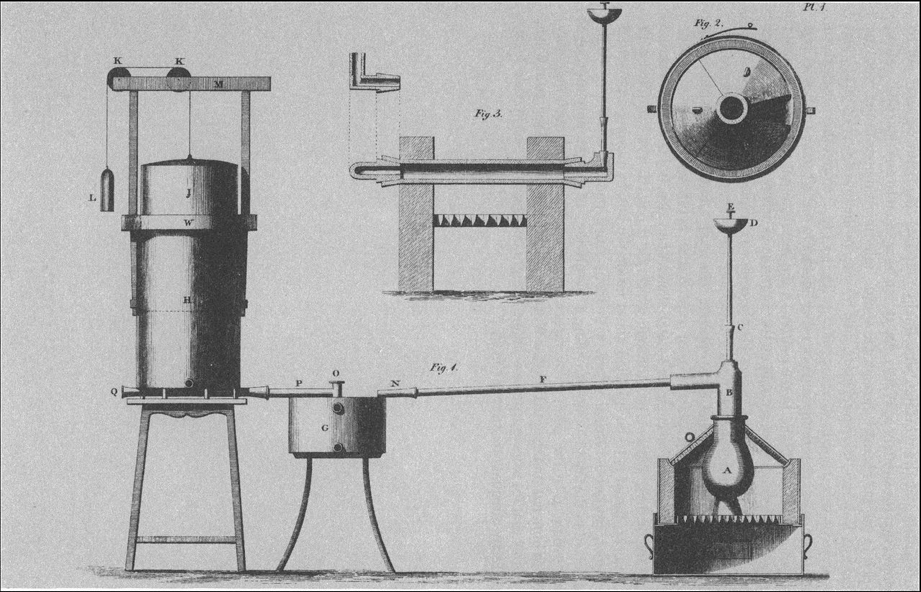
Some of the equipment designed by Watt for Beddoes in the mid-1790s. Source: Wikipedia
Some of the clinical work done at the Institution can be considered a forerunner of respiratory therapy. Beddoes gathered numerous case reports from his extensive network of physicians in Britain who were also using gas therapy. Methods of manufacture, storage, measurement, and inhalation of several gases were developed. James Watt and William Clayfield created extensive apparatus for these efforts; Watt had been working with Beddoes since the early 1790s.
So what would have happened if Beddoes and Davy had seized on the pain relieving properties of nitrous oxide and attempted to bring it into surgery? In addition to his suspect-to-the-crown political activities, Beddoes was a vociferous critic of the medical practice of his day and had a real concern for suffering patients both wealthy and poor. We can indeed imagine that he might have seized upon the possibility of pain-free surgery.
However, not being one himself, he would have needed one or more surgeons to participate in such experiments—just as William Morton would eventually collaborate with Dr. John Warren. Beddoes would probably have been further ostracized by fellow physicians if he teamed with surgeons, but that might not concern him. The real problem to overcome would be finding a surgeon willing to be ostracized by his peers.
By 1800 in England the medical profession consisted of several powerful organizations. The Barber-Surgeons’ Company, chartered in 1540, had become the Royal College of Surgeons. The apothecaries won independence from the grocers in 1618 and won independence from regulation by the London College of Physicians in 1704. These health care practitioners and others competed in an essentially free market.
As researchers later learned, nitrous oxide or a nitrous oxide/oxygen mixture were very useful in dental procedures or brief surgeries. The speed of surgeons in Beddoes’ day would have worked in tandem with those physiological properties of nitrous oxide inhalation by humans. Surgical procedures using the gas in 1800 would have faced two major problems already present: infection and blood loss. Despite those problems, the ability to relieve the pain of surgery might have increased the number of patients willing to go under the knife.
Proceeding along these radical lines would no doubt have increased the public ridicule and printed satiric attacks against the gas research beyond what really happened. Davy might have left for London anyway and been forced to disavow the work in order to further his own ambitions.
Britain’s years of fighting in the Napoleonic wars would have been a useful arena for pain relief during the many amputations performed. Like all nineteenth century wars fevers, typhus, dysentery, cholera, and so forth caused many if not most casualties, but bullet wounds also provided many sites for surgery. Ether anesthesia was finally used briefly by both sides in the Mexican-American conflict, and ether and chloroform more extensively by both Russia and Britain in the Crimean War of the 1850s. Both general anesthetics were also widely used by both combatants in the American Civil War.
During the decades between 1800 and Long’s 1842 surgeries in Georgia, nitrous oxide and ether became the agents of private recreational parties known as “frolics”. Public demonstrations by travelling showmen of the hilarious effects of nitrous oxide inhalation on audience members and by chemistry professors on university students were common. That these substances could also have serious medical use was an intellectual leap most could not make. The presence of mesmerists touring Britain, the Continent, and America and their wild claims only added to the aura of quackery.
What if Beddoes and Davy had attempted surgical anesthesia in 1799? We tend to think of the pain and suffering that might have been relieved in thousands of patients over the following four decades if they had. Yet the results could have been less salubrious. Failures would have been magnified by opponents of such radical experiments. Attacks from inside and outside the medical profession may have quickly stopped the work; other physicians and surgeons would have been reluctant to try the new procedures.
Crawford Long tried surgical anesthesia, but did not pursue or publicize his work. A local mentor cautioned him against further experimentation. Long’s location in the small town of Jefferson, Georgia, did not provide a place of open minds and innovation.
A few years later William Morton demonstrated the same procedure for one of the most prominent surgeons of the day, as well as others in the audience at a leading hospital in a city that already claimed itself the “Athens of America.” This context provided Morton with an instant support system to diffuse his “discovery.” Despite the ensuing debate among Morton, Wells, Jackson and Long about credit, the idea of surgical anesthesia found enough willing surgeons and patients to spread quickly. I suppose we can be thankful they did not have to overcome the notoriety that an effort four decades earlier might have created.
doi: 10.15763/JOU.TS.2015.4.1.01
Bibliography
Bergman, Norman A. The Genesis of Surgical Anesthesia. Wood Library-Museum of Anesthesiology, 1998
Davy, Humphry. Researches, Chemical and Philosophical; Chiefly Concerning Nitrous Oxide, or Dephlogisticated Nitrous Air, and its Respiration. Joseph Johnson, 1800
Jacob, Margaret C. and Michael J. Sauter. Why did Humphry Davy and associates not pursue the pain-alleviating effects of nitrous oxide? Journal of the History of Medicine 2002 April; 57: 161-176
Jay, Mike. The Atmosphere of Heaven: The Unnatural Experiments of Dr. Beddoes and His Sons of Genius. Yale University Press, 2009
Keys, Thomas. The History of Surgical Anesthesia. Krieger, 1978
Snow, Stephanie J. Blessed Days of Anaesthesia: How Anaesthetics Changed the World. Oxford University Press, 2008
Wright AJ. Humphry Davy’s small circle of Bristol friends. Middle East Journal of Anesthesiology 1995; 13(3): 233-277
Wright AJ. “I feel three quarters of immensity!” Satires of early nitrous oxide research. Bulletin of Anesthesia History 1996 Janu
